If you’ve ever delayed or avoided therapy because of insurance confusion, you’re not alone. One in five U.S. adults (20%) report putting off mental health care due to difficulties navigating health insurance or open enrollment decisions, according to our new survey.
For many Americans, choosing a health plan means relying on employer-sponsored coverage. However, determining whether mental health benefits will truly meet their needs isn’t always straightforward. Even as employers expand access to counseling benefits and absorb a significant share of rising premium costs, employees often struggle to make informed choices.
Confusing language and complex cost structures can leave many unsure if their health insurance will cover the care they need. Only 64% feel at least somewhat confident in their ability to choose health insurance coverage that they believe will meet their mental health needs. This report examines how guided, clear information can help people make informed choices to receive timely access to therapy.
Key takeaways
- Nearly one-third (32%) find copays, deductibles, and out-of-pocket costs to be the most confusing parts of choosing mental health coverage.
- One in five (20%) have delayed or avoided therapy due to insurance or difficulties with enrollment.
- Only 31% express strong confidence in their ability to select a health benefits and insurance plan that meets their mental health needs.
- 64% report being at least somewhat confident in their ability to choose a health insurance plan that covers their mental health needs.
Confidence gaps in selecting mental health benefits leave many behind
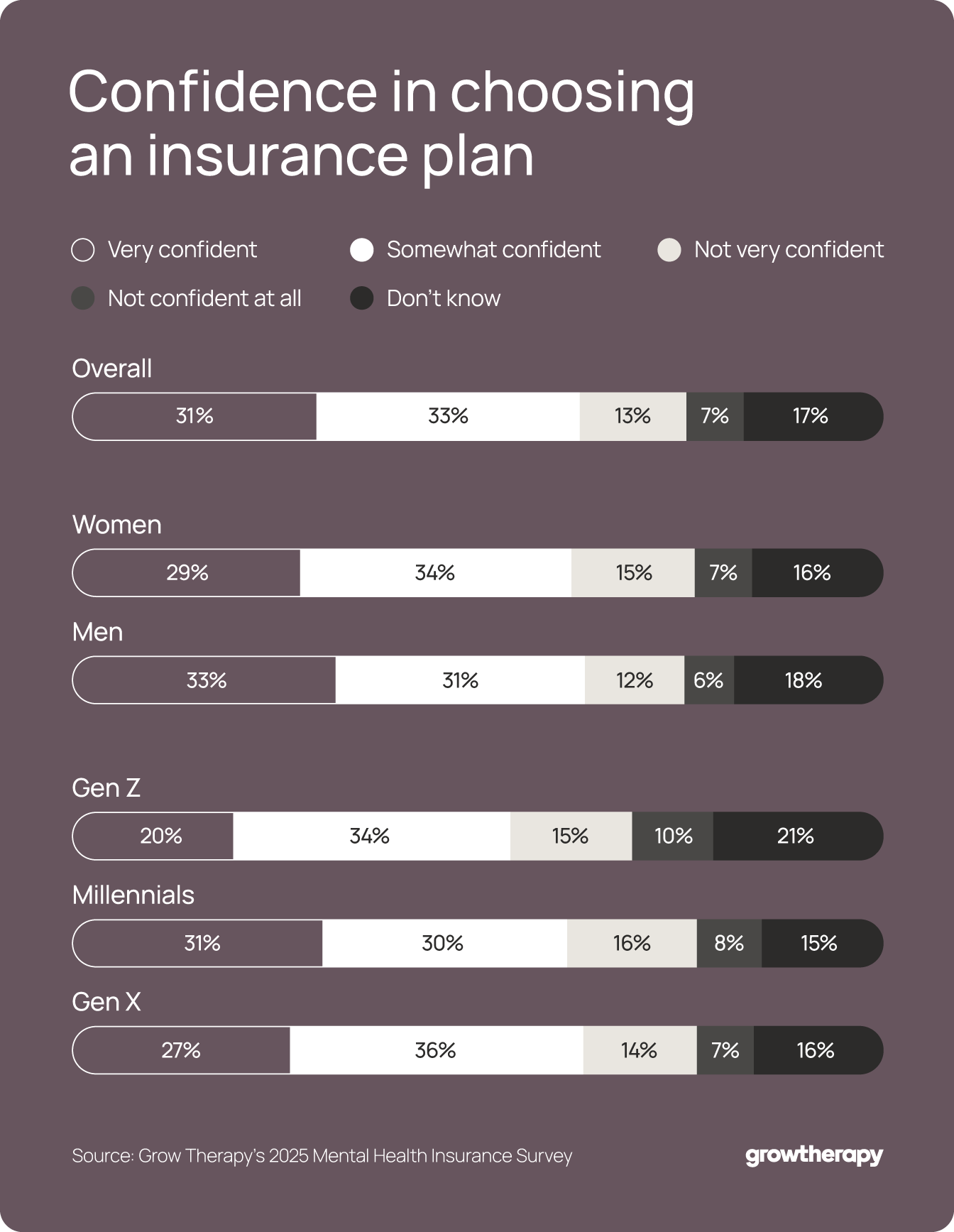
Even for people who have insurance coverage, understanding what’s actually covered remains a significant challenge. Less than a third (31%) of Americans say they feel very confident selecting a health insurance plan that supports their mental health needs, and that confidence differs across generations. Gen Z adults are the least likely to report high confidence (20%), with confidence improving slightly among Gen X (27%) and millennials (31%), showing that coverage literacy improves slightly with age. However, confusion still persists across all age groups.
These gaps matter. Nearly 1 in 4 (23%) U.S. adults experienced a mental illness in 2024 (over 60 million people), yet many employees still struggle to navigate their options. When people don’t understand or feel confident about their coverage, those most vulnerable may end up unable to find the right fit. Digital tools and clearer plan explanations can make navigating mental health coverage easier and help people feel more confident.
Cost confusion: The main barrier to selecting coverage
Cost confusion is the single biggest obstacle to confident decision-making: 32% of people say copays, deductibles, and out-of-pocket costs are the most confusing parts of coverage to understand during open enrollment. These factors make it difficult for employees to accurately predict the cost of therapy.
Many don’t understand that even when therapy is covered, high out-of-pocket costs — payments that aren’t reimbursed by insurance — can make a barrier to accessing care. The average deductible for single coverage — the amount you must pay for covered services before your insurance begins contributing — has risen by 43% over the past decade. High-deductible health plans (HDHPs) can also require thousands of dollars upfront. Nearly 29% of workers have these plans, and while some have access to Health Savings Accounts (HSAs) that let them use pre-tax dollars to offset these expenses, not everyone can contribute enough to meet rising costs.
Without transparent pricing or easy-to-understand health insurance summaries, many consumers don’t know what they’ll actually owe until after a claim is filed. This uncertainty can discourage people from seeking therapy — highlighting the importance of cost transparency in achieving equal access and timely care.
The impact of therapy delays on parents
Confusion over coverage for therapy can lead to delayed treatment. One in five Americans (20%) say they’ve avoided or postponed therapy because of insurance or open-enrollment challenges.
Notably, parents with children under 18 (26%) have struggled when trying to find affordable therapy for their children. A recent Grow Therapy Student Mental Health Report revealed that nearly 1 in 5 parents said high costs, insurance limitations, or long waitlists made it difficult to get mental health support for their child — even with coverage.
Some of this stems from not knowing about benefits that could make therapy more affordable. Licensed therapist Monica Randle explains:
“If an individual would like to see a provider who is outside of their insurance network, there is an option to use Out-Of-Network (OON) benefits… The individual may receive partial reimbursement for treatment rendered in this case. In cases where a relationship has already been established, providers may seek to obtain a Single Case Agreement (SCA) from the insurance carrier… This option may be beneficial in situations where a client has a change in healthcare coverage.”
— Monica Randle, LPCC, LPC
These lesser-known coverage options can make a difference for families navigating complex benefits. The good news is that clearer plan information and the right resources can simplify this process, helping people understand their coverage and get connected to care sooner.

Clear comparison charts and expert guidance would make choosing easier
Nearly 40% of Americans say that clear, visual comparison charts would make it easier to choose a plan. Almost 53% want expert assistance or step-by-step guides to help them sort through their options.
Grow Therapy offers resources like our Paying for Therapy Guide, cost estimator tool, and transparent in-network provider listings — all designed to make plan selection easier. These tools are especially valuable for younger adults and working parents looking for digital support to help them find therapists who accept their insurance.

What this means for you
Mental health coverage has come a long way, but confusion continues to hinder access. Cost complexity, unclear provider networks, and varying confidence levels leave too many people unsure where to start.
The good news is that the tools people want already exist. If you’re comparing plans during open enrollment, taking the time to understand your mental health coverage now can make a real difference. Grow Therapy’s insurance check tool helps to see whether a plan is accepted and estimates out-of-pocket costs. Many clients with employer-sponsored insurance plans average low fees per session — though exact pricing always depends on the individual plan.
Take the next step in your mental-health journey and get matched with a licensed Grow Therapy therapist today.
Methodology
The survey was conducted by YouGov for Grow Therapy. The survey was fielded between October 24-28, 2025. The results are based on 2,424 completed surveys. Data is weighted, and the margin of error is approximately +/-3% for the overall sample with a 95% confidence level.

